When Prevention Works, Children Live: Is Nigeria Ready to Scale a Malaria Vaccine That’s Cutting Child Deaths in Half?
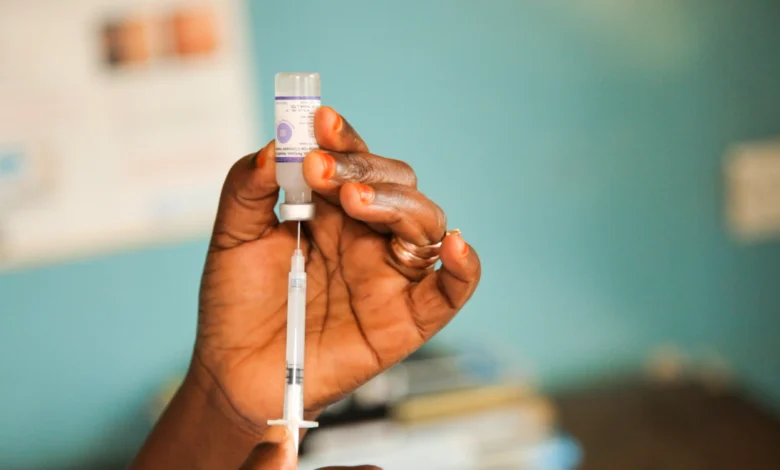
In Kebbi State, northwestern Nigeria, the rollout of the R21 malaria vaccine is delivering measurable progress for a child’s most fundamental right: the right to survival.
One year after the vaccine was integrated into the routine immunisation schedule, more than 200,000 children have received at least one dose. Health officials report hospital malaria cases have dropped by about 50% in selected facilities, and under-five mortality has fallen significantly within ten months.
For a state with one of the highest malaria prevalence rates among children under five, this shift is more than statistical. It means fewer hospital beds filled with critically ill children, fewer frantic midnight journeys to clinics, and fewer small graves dug too soon. Nigeria carries 27% of the global malaria burden, making progress here globally significant.
This momentum has been backed by coordinated efforts from state health authorities and partners including Gavi, the Vaccine Alliance, UNICEF, and World Health Organization. Community outreach, media campaigns, and integration into routine immunisation schedules have helped drive uptake.
But survival gains must be sustained. Some children have yet to complete all recommended doses, and continued investment in cold chain systems, rural access, and caregiver education remains critical.
Expanding coverage, strengthening follow-up systems, and pairing vaccination with mosquito control and early testing will determine whether this early success becomes long-term transformation.
The early results raise a pressing question: if we now have a tool that saves children’s lives at scale, how quickly and how widely will we use it?





